Pediatric Trauma
4. Pediatric Trauma Assessment
4.6. Thoracic Injuries
In children, thoracic injuries are associated with a high mortality rate. It is known that chest injuries cause 25% trauma deaths, mostly due to respiratory failure (Shorr et al, 1987). The greater elasticity of the ribs and sternum makes fractures less common than in adults, but there is a higher rate of energy transfer to the underlying structures (Box 7). Sternal fractures should raise the suspicion of myocardial trauma, pulmonary contusion, and great vessel injury.
BOX 7: Frequency of thoracic injuries in pediatric trauma
- Pulmonary contusion/laceration (53%)
- Pneumothorax/hemothorax (38%)
- Rib/sternum fractures (36%)
- Other lesions
- Cardiac (5%)
- Diaphragm (2%)
- Major blood vessels (1%)
From: Kassis K, Grady M. Trauma and burns in Johns Hopkins. In: Gunn VL, Nechyba C, eds. The Harriet Lane handbook: a manual for pediatric house officers, 16th ed. St. Louis: Mosby, 2002:79-94
Pulmonary contusions are the most frequent type of injury occurring with thoracic trauma. They are often missed because the initial clinical findings can be subtle. A pulmonary contusion is essentially a bruise of the lung that leads to alveolar hemorrhage and interstitial hemorrhage and edema. The severity is related to the extent of lung tissue involved. Clinical signs and symptoms include soft tissue marks on the chest, tachypnea, use of accessory respiratory muscles, and hypoxia. Continuous pulse oximetry is needed, as well as blood gas evaluation to assess the degree of PaO2 reduction and PaCO2 increase whenever possible. It is possible that decisions on ventilator management will need to be made clinically based on chest wall movement, breath sounds, and oximetry. Treatment of lung contusions consist of oxygen therapy, close monitoring, and possibly endotracheal intubation with positive end-expiratory pressure (PEEP) to help tamponade bleeding.
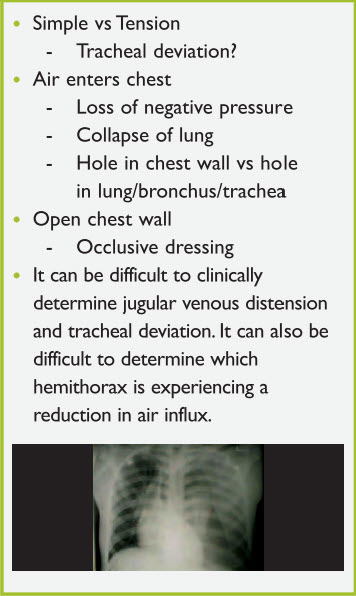
In all pneumothoraces, air enters the pleural space resulting in loss of negative pressure and lung collapse. Air may enter either through a hole in the chest wall or a hole in the lung, bronchus, or trachea. An open pneumothorax exists when there is an opening in the chest wall. Immediate treatment of such a condition consists of applying an occlusive dressing. Pneumothorax can either be simple or under tension. Assessment of the trachea helps differentiate between the two. Tension pneumothorax is a clinical diagnosis made by tracheal deviation away from the side of the pneumothorax, absent breath sounds, hypotension, and possibly distended neck veins. In young children, it may be difficult to clinically determine jugular venous distension and tracheal deviation. Tension pneumothorax is a clinical diagnosis requiring immediate needle decompression at the second intercostal space along the mid-clavicular line or placement of a chest tube in the fourth to fifth intercostal space along the mid-axillary line (Figure 8).
Figure 8. Pneumothorax
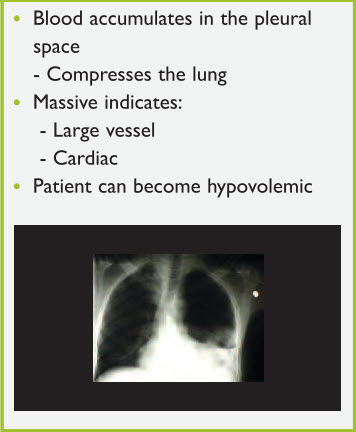
Hemothorax occurs when blood accumulates in the pleural space, which can then compress the lung. A massive hemothorax indicates a large lung injury with potential involvement of large vessels (Figure 9).
Figure 9. Hemothorax
Draining the blood from the chest with a chest tube (posterior location) and treating the hypovolemia are the keys to therapy.
Pericardial tamponade presents when fluid accumulates in the pericardial sac. In trauma, this fluid is blood and usually develops over minutes to hours. This fluid causes a restriction on the myocardium leading to decreased cardiac output and hampered venous return. Clinically, Beck's triad suggests pericardial tamponade: reduced pulse pressure, neck vein distension, and muffled heart tones. Arrhythmias can be present including bradycardia, pulseless electrical activity (PEA), and asystole. The treatment includes pericardiocentesis and intravenous fluids. Clinical suspicion should arise when a penetrating trauma to the trunk has occurred. Look for soft tissue marks, such as entry site of a penetrating object and bruises across the chest wall.