Pediatric Trauma
3. Response to A Disaster
oBjectives
- Emphasize the importance of safety and transportation of the wounded.
- Review the patient classification process according to the severity of the trauma and the available resources.
What Elements should a Plan for a Disaster Situation Include?
First, assume that the health care facility, wherever its location, will need to function alone until outside help arrives. It is, therefore, important to have a notification system to call in extra personnel.
It is always essential to use a triage (injured patient classification) system and to prepare adequate treatment areas to handle the influx of patients. Free up operating rooms and intensive care beds and carefully check on all available supplies (blood, medications, communication equipment). Always consider that decontamination procedures may need to be implemented as indicated. It is also necessary to ensure security in the emergency setting and to start transferring the injured people according to the priorities established through the classification process and the available resources. A public information center will be needed to distribute information to media and families. Annual drills help familiarize the staff with the disaster plans, as well as provide feedback to finetune the plans.
Available Personnel
Having a list of available personnel and appropriate means to contact them is a critical preparatory step in the face of a disaster. Arrange a central communication system that can activate a call-up roster to ensure the timely arrival of this help.
Once the personnel are at the medical facility, it becomes important to organize this labor force and provide job descriptions. A military model has been adapted to the hospital setting and is referred to as the Hospital Incident Command System (HICS). HICS has become the standard for health care disaster response and offers predictable management schemes, flexible organizational charts, prioritized response check-list, accountability of position function, and common language when communicating with outside groups.
CASE 1:
Your health care unit is sent to a neighborhood to see a child who has suffered a fall. You find an 8-year-old boy lying on the grass near a big tree. An adolescent tells you that she saw him fall from the tree when he was at a height of about 30 feet. Nobody has moved him.
Initial assessment shows that the boy is responding only to painful stimuli. Breathing is superficial with audible snoring. The skin is pale, with mild cyanosis. Respiratory rate is 12 breaths per minute; heart rate is 130 beats per minute.
The skin is cold, radial pulse is weak, and capillary refill is >3 seconds. Pupils are equally dilated and are reactive to light. Air influx cannot be detected through auscultation in the right hemithorax and is diminished in the left. Oxygen saturation is 82%.
He has broken teeth and a swollen nose, with moderate hemorrhage. The abdomen is stiff on palpation. The right leg is swollen, with evident deformity to the femur.
- Based on initial assessment and type of trauma, what are the most probable injuries in this boy?
- Analyze the initial stabilization measures and pre-hospital management of this child.
Specific Pediatric Equipment needs
Specific equipment must be available in disaster emergency situations involving children. Box 1 displays a list of recommended equipment.
BOX 1: Recommended equipment for pediatric emergencies in disaster situations
Airway Management
- Oxygen source with flow-meter
- Simple face masks – infant, child, adult
- Pediatric and adult masks for assisted ventilation
- Self-inflating bag with 250 cc, 500 cc, and 1000 cc reservoir
- Wall suctioning device or suctioning machine
- Suction catheters – Yankauer, 8, 10, 14F
- Oropharyngeal airway tubing (infant and adult sizes)
- Nasal tubing – infant, child, and adult sizes 1-3
- Optional for intubation
- Laryngoscope handle with batteries
- Miller blades – 0, 1, 2, 3
- Endotracheal tubes, uncuffed – 3.0, 3.5, 4.0, 4.5, 5.0, 6.0, cuffed – 7.0, 8.0
- Intubation guides – small, large
- Adhesive tape to secure endotracheal tube
Intravascular Access or Fluid Management
- IV catheters – 18, 20, 22, 24-gauge
- Butterfly needles – 23-gauge
- Intraosseous needles – 15- or 18-gauge
- Boards, tape, tourniquet IV
- Pediatric drip chambers and tubing
- 5% dextrose in normal saline and half normal saline
- Isotonic fluids (normal saline or lactated Ringer’s solution)
Miscellaneous
- Blood pressure cuffs – premature, infant, child, adult
- Nasogastric tubes – 8, 10, 14F
- Sphygmomanometer
- Splints and gauze padding
- Rolling carts with supplies such as abundant blankets
- Warm water source and portable showers for decontamination
- Thermal control (radiant cradle, lamps)
- Geiger counter (if suspicion of radioactive contamination)
- Personal protective equipment (PPE)
Monitoring Equipment
- Portable monitor/defibrillator (with settings <10)
- Pediatric defibrillation paddles
- Pediatric ECG skin electrode contacts (peel and stick)
- Pulse oxymeter with reusable (older children) and non-reusable (small children) sensors
- Device to check serum glucose and strips to check urine for glucose, blood, etc.
Among the recommended equipment, elements for proper airway management in children are crucial. A major challenge of any disaster response is gathering, organizing, and moving supplies to the affected area. Resource management within the hospital and other facilities or agencies may prove to be a decisive factor in whether a mass casualty event can be handled or not.
Communication
A very important aspect during a disaster situation is the ability to communicate, not only with others in the community but also among the medical personnel involved in responding to the situation. A coordinated response is needed in order to adequately handle a large influx of patients. Ideally, personal radios or cell phones should be available, so that the personnel involved in health care management communicate with each other and with the central command leader. The same applies to other areas (administration, security, maintenance).
Scene Safety and Transport
Most physicians are not trained in onscene rescue efforts. In general, local police, firefighters, and hazmat teams are the best to initially approach and control a disaster scene. However, in confined spaces, triage may need to be set up in the field and this may put the health care providers close to the disaster location.
What are the risks involved at the disaster scene?
Risks at the actual disaster scene vary according to the nature of the disaster. These include: structural instability and further collapse, fires, carbon monoxide, cyanide, dirty bombs, contamination with biologic material, and infectious agents. Other potential hazards in confined spaces include: poor air quality, airborne pollutants, toxic gases, an explosive/flammable atmosphere, and insufficient oxygen concentration (Box 2).
BOX 2: Risks at a scene of a disaster
- Structural instability and further collapse
- Fires, carbon monoxide, noxious gases such as cyanide
- Heavy dust load; insufficient oxygen
- Dirty bombs: chemical, radioactive
- Biohazard: sewage, body fluids, blood exposure
- Infectious agents
Ideally, patients will be promptly transported to a local medical clinic or hospital. The initial response at the scene of a large disaster, once the patient has been rescued, includes airway support, spine immobilization, and oxygen delivery. The increased neck flexion that occurs from the large head of small children on a backboard can be addressed with either a scooped-out head area on the backboard or with a small roll of cloth placed under the shoulders to elevate the trunk (Figure 1). Immobilization on a backboard is primarily expected to protect the spine during transport and facilitate transport. It is important to get the child off the backboard within a couple of hours.
Figure 1. Scene Immobilization
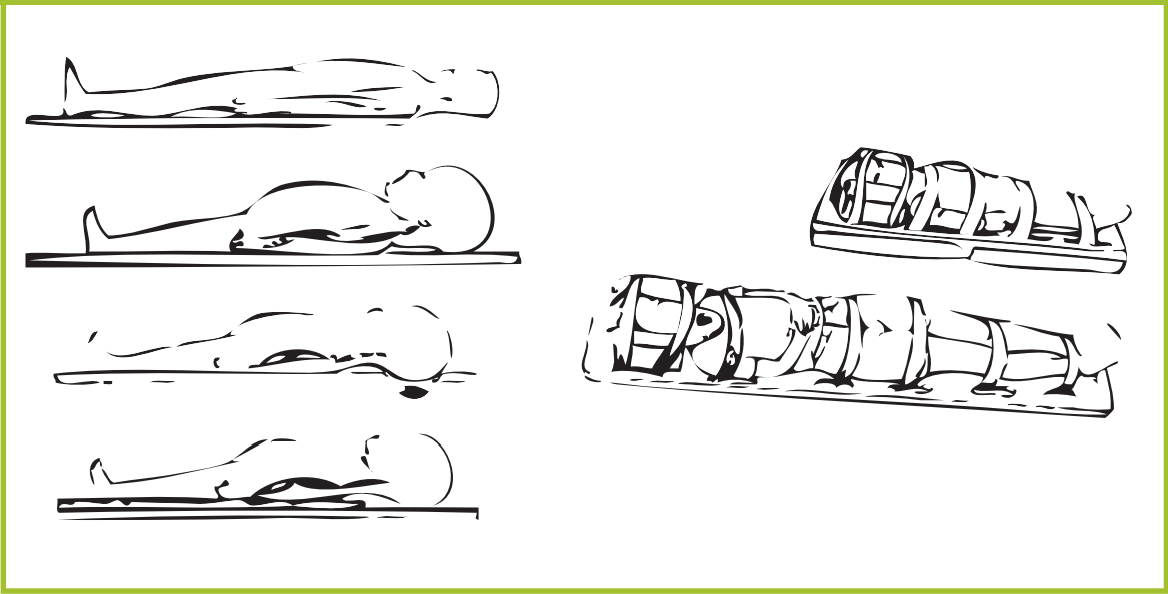
Keeping the airway open during transport of the traumatized child is a top priority. Airway support can be adequately maintained with bag-valve-mask ventilation (BVM). Intubation in children prior to transport is not necessary and has not been shown to improve outcome. In fact, endotracheal intubation can lead to delayed transport and increased morbidity due to improper tube placement or possible dislodgement of the tube during transport. A large study in children compared endotracheal intubation versus BVM in the pre-hospital setting. This study included 830 patients below age 13, randomly assigned to BVM or endotracheal intubation. Results showed that there was no advantage in placing an endotracheal tube (ETT) prior to transport to a hospital (Gausche et al., 2000). This adds to the risks that may arise from improper ETT placement. Therefore, proper BVM technique remains one of the most important skills to teach and review with local first responders to a disaster situation (Figure 2).
Figure 2. Bag-valve-mask ventilation
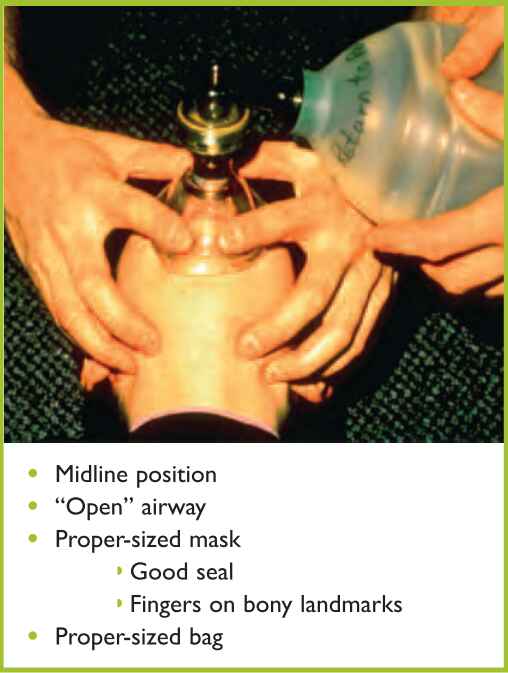
Injured individuals with high morbidity or mortality risk should be promptly transported. The highest level of pediatric health care is needed for falls, fires, explosions, blunt injuries, and penetrating injuries (Box 3).
BOX 3: High-risk pediatric injuries
- Falls from more than 6 m
- Fires: burns and asphyxia or highrisk burns (>10% second-degree or >5% third-degree or any burn with airway involvement)
- Explosions
- Blunt trauma: Significant injury with physiologic compromise (tachycardia with at least two signs of hypoperfusion or hypotension for age or altered mental status or spinal cord injury with neurological compromise)
- Penetrating injuries: shot, stabbing